Our Victoria TMJ Physiotherapists Jennifer Kolot and Ruan LeRoux have received post secondary training to treat jaw and TMJ pain & problems. Chronic or acute TMJ dysfunction can respond very favourably to specific and effective Physiotherapy treatments. You don’t have to live with it. TMJ Physiotherapy can help! Our Shelbourne Physiotherapists look forward to helping you recover. The goals of physiotherapy treatment are to reduce pain and inflammation of the TMJ, and to improve TMJ movement and function. Treatment focuses on both the TMJ and other body parts that are contributing to the problem. Excessive chronic tension in the muscles connected with and surrounding the TMJ can cause not only local pain perception in the area of the jaw itself, but can also set up pain referral patterns (through trigger points) causing regular experiences of headaches, migraines, involuntary teeth grinding, gum or tooth related pain and even ringing in the ears (tinnitus). We will be happy to work in conjunction with your dentist to provide the most comprehensive treatment possible.
What is the Temporomandibular Joint (TMJ)?
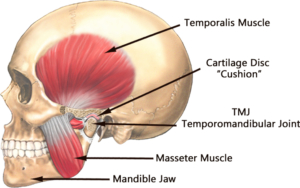 The TMJ or temporomandibular joint is the formal anatomical name given to the jaw joint, where the mandible bone (which forms the lower jaw) meets the skull (at the temporal bone). The TMJ is a complex hinge joint that is made up of several parts; the lower jaw (mandible) and the socket (temporal bone). In between the mandible and the socket is a disc. This disc allows the jaw joint to glide smoothly when opening and closing and this joint is held in place by muscles and ligaments. There are a number of small but remarkably strong muscles which attach to and surround this joint and which are involved in talking, yawning, drinking, smiling, eating/mastication (i.e. chewing) as well as other facial movements involving the jaw. The TMJ which opens 2,000-3,000 times per day is the most frequently used joint in the body. Most people are only aware of this joint when it becomes painful. It can be painful as a result of injury, inflammatory diseases, poor posture and habits or growth disorders.
The TMJ or temporomandibular joint is the formal anatomical name given to the jaw joint, where the mandible bone (which forms the lower jaw) meets the skull (at the temporal bone). The TMJ is a complex hinge joint that is made up of several parts; the lower jaw (mandible) and the socket (temporal bone). In between the mandible and the socket is a disc. This disc allows the jaw joint to glide smoothly when opening and closing and this joint is held in place by muscles and ligaments. There are a number of small but remarkably strong muscles which attach to and surround this joint and which are involved in talking, yawning, drinking, smiling, eating/mastication (i.e. chewing) as well as other facial movements involving the jaw. The TMJ which opens 2,000-3,000 times per day is the most frequently used joint in the body. Most people are only aware of this joint when it becomes painful. It can be painful as a result of injury, inflammatory diseases, poor posture and habits or growth disorders.
TMJ Disorders affect 5 out of every 100 people and they can be quite debilitating
What are the Symptoms of Temporomandibular Joint Dysfunction (TMD) ?
 TMD is often associated with postural dysfunction and accompanied by neck pain and headaches. TMD can cause significant functional limitations ranging from inability to eat hard food, yawn comfortably to chronic intractable pain. TMD occurs at a higher frequency for females as well as those who have experienced a whiplash injury. TMD can present as a single symptom or a cluster of symptoms which may include:
TMD is often associated with postural dysfunction and accompanied by neck pain and headaches. TMD can cause significant functional limitations ranging from inability to eat hard food, yawn comfortably to chronic intractable pain. TMD occurs at a higher frequency for females as well as those who have experienced a whiplash injury. TMD can present as a single symptom or a cluster of symptoms which may include:
- Clicking sensation, grinding, popping, locking or deviation of the jaw during opening
- Pain, tightness or tenderness in the jaw joints and facial muscles
- Difficulty closing or opening the mouth comfortably
- Experience dizziness or frequent neck & headaches
- Change in the way the upper and lower teeth fit together
- Hearing loss, Ear pain, fullness of the ears and ringing in the ears (Tinnitus)
- Reduced ability to fully close or open the mouth
- Fibromyalgia
- Muscle spasms in the face, head or neck
What are the Causes of Temporomandibular Joint Dysfunction (TMD)?
The pain and tenderness of TMJ dysfunction can be caused by the disc in the TMJ joint moving out of place and causing pressure on sensitive structures around the joint. There can be a number of causes and frequently it can be a combination of these rather than a single cause. The most common causes of TMD include:
- Prolonged mouth opening e.g. dental surgery
- Clenching or grinding of the teeth (bruxism)
- Poor cervical posture leading to strains or overuse of muscles in the face and neck
- Removal of wisdom teeth
- Rheumatoid Arthritis
- Poor habits such as excessive gum chewing, cheek biting and fingernail biting
- Lack of restful sleep
- Poor alignment of teeth or dental problems
- Wear and tear of the cartilage inside of the joint
- Poor diet
- Increased sensitivity to pain linked to stress
- Alignment or structural problems present since birth
- Trauma to the jaw area e.g whiplash, fractures, concussion, sports injury or motor vehicle accident
- Emotional Stress and inability to relax
TMJ Physiotherapy Treatment Research
Using Physical Therapy to treat temporomandibular disorders: A cohort study
How Physiotherapy can help with temporomandibular dysfunction (TMD)
Temporomandibular disorders. Orofacial Pain: Guidelines for Assessment, Diagnosis, and Management.
Clinical Examination of the Orofacial Region in Patients with Headache.
Tension-Type and Cervicogenic Headache: Physiology Diagnosis, and Management
International Classification of Headache Disorder
Home-exercise regimes for the management of non-specific temporomandibular disorders.
Screening for psychosocial risk factors in patients with chronic orofacial pain.
